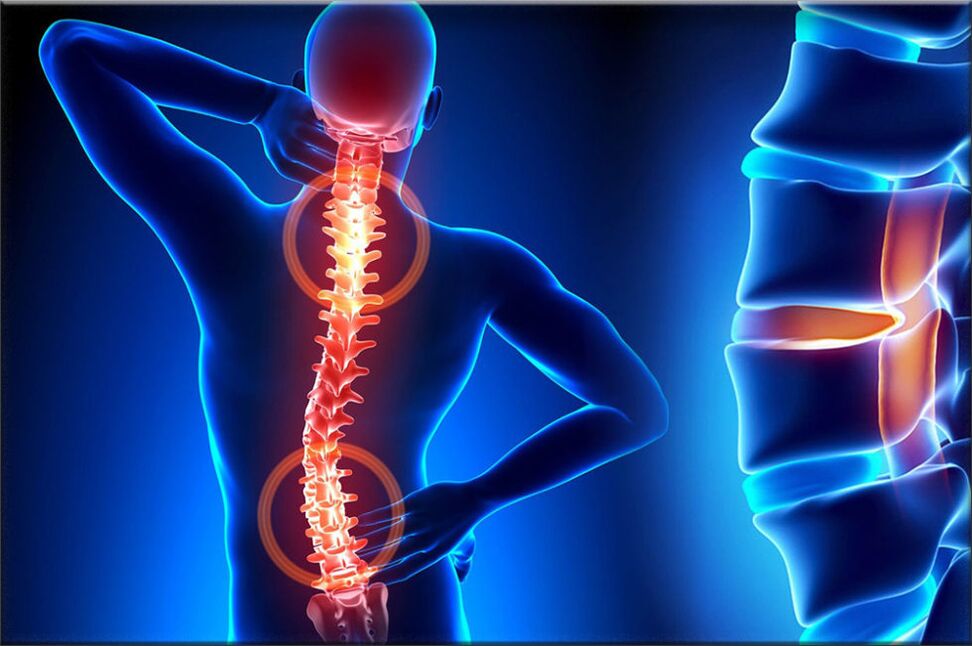
Osteoporosis is one of the most common pathologies of the musculoskeletal system, manifested as a result of a complex of dystrophic changes in the cartilage of the vertebra, in the course of this pathology, the intervertebral discs of the column. Life is often affected. The structures, which are the buffered cartilage discs, provide flexibility and also allow the human spine to move, i. e. they provide movement.
With bone necrosis, a number of processes take place causing degeneration of the vertebral disc, as a result they begin to lose elasticity and reduce flexibility, and at this point the disc becomes quite flat. The distance between the two discs gradually decreases, simultaneously compresses the nerve ends and blood vessels and causes severe pain. The pinched site of the nerve node begins to swell, leading to increased pain and even more compromise.
During the development of osteonecrosis, muscle structures and most organs of the body are often involved in this pathological process. This is due to the fact that in the course of maximum violation of the nerve bundle, blood circulation and peristalsis of muscles and organs are disturbed. For example, the most common bone necrosis disease is cervical bone necrosis, which is accompanied by pain in the back of the head, nausea, dizziness, impaired vision and often tinnitus. The disease has become quite "young": a century ago, osteonecrosis was a disease of the elderly, and young people are also susceptible today.

The most vulnerable are those with a severe decrease in the body's metabolism and hormonal levels, as well as those with disorders of vascular properties. This is due to the fact that these diseases cause the disc oxidation disruption. If qualified, there is no timely treatment, the anatomically compressed disc edges will protrude beyond the limit of the spine, thereby destroying the nerve bundles.
Because at this time, the patient is at risk of a herniated disc. The main, significant cause of osteonecrosis is uneven distribution of load onto the spine, resulting in a change in cartilage structure at points of excessive stress. The nature of this disease depends on the stage and extent of the damage to the affected disc. The discs change with age, just like our hair. Major trauma or fracture of the spine can affect how they work. Casual clothing and certain types of vibrations can also speed spinal degeneration. In addition, there is a lot of evidence that smoking increases the rate of spinal degeneration. Scientists have also found connections among family members, highlighting how quickly genetics plays a role in change.
The disease can also be triggered by many factors:
- wounds, bruises;
- spinal muscular dystrophy;
- stooping and scoliosis;
- lift the weight;
- stretching time in one position;
- metabolic disease;
- lack of trace elements and vitamins - manganese, magnesium, zinc and vitamins D and F;
- genetic predisposition;
- physical overload;
- sedentary lifestyle;
- radiation background;
- freezing;
- congenital dystrophy;
- asymmetric work of the muscles of the spine;
- stress, depression.
These causes of osteonecrosis are only scientists' assumptions, the direct cause of the disease, science has not yet found it and we are only talking about the risk factor.
First perioddevelopment - is characterized by early proliferation of the inner nuclear spinal cord (the nuclear spinal cord of the eccentric disc, located next to the dorsal part of the vertebrae).
Second stageCharacterized by the appearance of instability of the spinal segment. The pathological substrate is represented by the fibrous nucleus of the affected disc with disassembled and fragmented degenerative processes of the posterior longitudinal ligament, the pathological movements between the vertebrae developing.
Ky autumn threedevelopment of the disease - complete damage to the disc, with the appearance of "herniated disc" - dislocation and escape of the myeloid fragments outside the disc space.
If the disease had reached its third stage, then the devastating process was irreversible and could lead to profound disability.
Types of bone necrosis
Progression of bone necrosis is slow, with exacerbations due to spinal injuries, exercise, weight bearing, etc. v. Clinic depends on the location of the lesion.
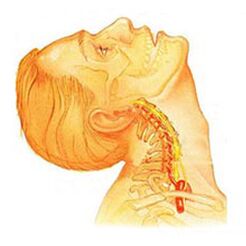
Cervical spine tumorsthere are local and remote symptoms of progressive forms - with large root domination, that is, it contributes to the development of severe lens pain. Symptoms of osteonecrosis of the cervical spine are accompanied by varying degrees of dysfunction, sometimes manifested in a sudden restriction of cervical spine mobility and functional masses. Headaches can be both prolonged and paroxysmal when irradiated to the inter-vertebrae or shoulder area. In the acute phase, the patient is diagnosed with neck pain, which interferes with and limited movement of the head and neck. In addition to severe discomfort, pain syndrome can be accompanied by dizziness, insomnia, pain, loss of appetite, depression, eye and pharyngeal diseases.
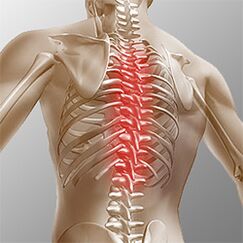
Osteonecrosis of the chest. . . Clinical manifestations are due to local damage and destruction of the root structure of the nerve. Chest necrosis has a pronounced pain syndrome, which can be of a chronic or acute nature of back pain with chest discomfort and limited muscle contraction, up to right speech atrophy. Chest pain can manifest as diffuse, intercostal, and neurological. Palpation enhances the ability to rotate the shaft of the vertebral body. The disorders correspond to the degree of root stimulation from Thl1 to Thl2, and can manifest themselves with angina attacks, reflected in liver and gastrointestinal dysfunction. Genital and genital system disorders often occur. The patient noted a marked decrease in sensory disorders such as paresthesia, superficial and deep sensitivity.
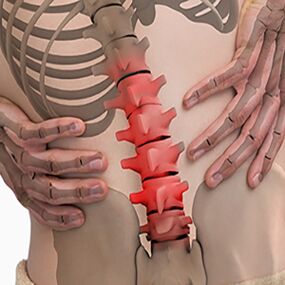
Lumbar necrosis. . . It is characterized by abdominal reflex and dysfunction of the lower extremities. During the development of neurological disorders, muscle weakness in the legs and pelvic organ dysfunction may occur. Osteonecrosis is characterized by an assessment of damage during sitting. The more advanced the lumbar vertebrae development stage, the shorter the time the patient can sit. Lumbar forms are characterized by chronic and acute back pain, spasm of the spinal muscles, and secondary myofascial syndrome. The pain spread down the buttocks and anus.
Depending on the localization of the pathological process of osteonecrosis, the disease can lead the patient to a violation of superficial sensitivity (touch, heat). Also characterized by altered reflexes (e. g. , no Achilles reflex), muscle weakness, muscle tone disturbances, autonomic disorders (pallor, erythema, nail nutrition changes, hypothermia in the distal limbs), sphincter dysfunction and sexual dysfunction.
Clinical image
DiagnoseBegin with a complete history and physical exam. The doctor questioned how the symptoms and diseases interfere with the patient's daily activities. In addition, the specialist is also interested in identifying sites and activities that emphasize or reduce pain levels.
The doctor then examines the patient, examines the position and range of motion of the spine, and then determines what movements are causing the pain. Skin sensitivity, muscle strength and reflexes were all tested equally. Based on your medical history and physical exam, the doctor determines which techniques will help.
X-rays rarely help diagnose, no more than 30% of X-rays show abnormalities in the early stages of disease development.
However, if the symptoms are severe and the disease is already in the second or third stage, defects can be seen in one or more disc in the picture. They can be penetrated by the bone-forming substances between the vertebrae and the joints.
If additional information is required, magnetic resonance imaging is prescribed. MRI is used to view the soft tissues of the body. This is useful if the core of the tissue absorbs water or if there are cracks inside the disc. An MRI scan can show problems in other soft tissues, such as spinal nerves.
Disk imaging can assist with diagnosis. This test is performed using a contrast agent, which is injected into one or more discs respectively. Later viewing on x-rays provides useful information about the condition of the disc.
Treatment of osteonecrosis, depending on the breed
Non-surgical treatment of bone necrosis
Whenever possible, doctors prefer non-surgical treatment. The most important thing in non-surgical treatment is to relieve pain and other discomfort so that the patient can return to the most comfortable standard of living possible.
Doctors rarely prescribe bed rest to patients with bone necrosis problems. Patients are encouraged to be physically active when pain is not a concern. If the symptoms are severe, a few days of bed rest can be prescribed.
When the spine is displaced, an elastic belt is sometimes prescribed, worn for no more than 2-4 days to avoid atrophy of the back muscles.
Chiropractic sessions help to reduce the severity of osteonecrosis.OsteopathNot only diagnose the problem area, but also relieve pain in 1-2 doses, reduce the general condition of the body and "tighten" the internal organs.
Patients may be prescribed medication to control symptoms and to continue normal activities for a long time. If symptoms continue to restrict the patient's activities, the doctor may usually recommend an epidural steroid injection.
Steroids are powerful anti-inflammatory drugs that help relieve pain and inflammation. Nonsteroidal anti-inflammatory injections are injected into the space around the spinal roots of the spine. This site is called the epidural space. Some doctors inject steroids on their own. However, it is often combined with other medications. Basically, steroids are prescribed only when other drugs are ineffective, but osteopathy is almost always effective.
In addition, patients often work with physiotherapists. After assessing the patient's condition, the therapist prescribes exercises to reduce symptoms. The exercise program is intended to improve flexibility and is useful for abdominal and back muscle training to allow movement with minimal pain.
Surgery
People with bone necrosis problems usually do not need surgical treatment. In fact, only 1-3% is functional. Surgeons appoint non-surgical treatment, namely cranial osteopathy, as a rehabilitation therapy, at least 3 months before considering surgery. If after 3 months of non-surgical treatment there is no result, then there is a basis to indicate surgery.
Basic surgical procedures
Evisceration
The procedure is to remove part or all of the disc in the lumbar region. Surgeons usually perform surgery through an incision in the lower back area. Before surgery to operate a herniated disc, some of the disc must be removed.
Today, surgery has mastered minimally invasive technique just a small incision in the lumbar region. Proponents of this method claim that it is safe. They also believe that the procedure prevents scarring around nerves and joints and helps patients recover faster.
Unify
This is an intervention that joins two or more bones into one, preventing the ends of bones and joints from being worn out.
Rehabilitation
The doctor may recommend that the patient see a physical therapist several times a week for 4-6 weeks. In some cases, the patient needs extra help.
The first year of treatment is needed to control symptoms. The therapist will work with you to find positions and movements that help relieve pain. Heat, cold, ultrasound and electrical stimulation can be prescribed for pain relief and muscle spasm. Massage or specialized forms of soft tissue movement may also be used. These procedures help the patient perform the movements easily.
Typically, the adjustment of treatment helps restore the sensitivity of the nerves and spinal muscles, reduces pain and improves mobility.
The main goal of therapy is to teach patients how to use them to prevent future problems. A series of exercises will be advised to improve flexibility. The patient will also be given a strategy to help in case of symptoms recur.
Each person should learn about and consider different types of osteonecrosis in order to prevent the development of the disease for themselves and loved ones. After all, the treatment of destroyed vertebrae is not possible, therapy aimed at relieving pain symptoms and achieving long-term remission. You also need to remember a simple yet effective rule:the best cure is prevention. . .
Prevention of bone necrosis
Prevention is quite simple - it's a healthy diet, regular muscle activity, a daily morning warm-up, a healthy and active lifestyle and a monthly visit.chiropractic treatment sessionsto correct and eliminate musculoskeletal stress. Following these rules is enough to never face the aforementioned problem and avoid terrible symptoms and lifelong treatment.






























