Cervical spondylosis is a disease in which the vertebrae and discs are affected. Cervical osteosarcoma refers to pathological deformation of the back. Intervertebral disc-related changes were observed at the age of 20. At the same time, they became more load-sensitive, less elastic, and lost lubricating fluid.
Usually, the pathology occurs in the elderly, but now the incidence in children and adolescents has increased significantly. Neurologists identify cervical osteonecrosis using the latest diagnostic studies. After a clear diagnosis, complex therapy is carried out with the most effective drugs, physiotherapeutic procedures and innovative methods of physical rehabilitation.
The name of the disease consists of two Greek terms "osteon" (bone) and "chondros" (cartilage). Cervical fibroids begin with changes in the central part of the disc. The disc loses moisture, reduces in size, this leads to convergence of the vertebral bodies and invasion of nerve roots with vessels. The vertebrae receive nutrients from the surrounding tissues, causing harm to the body. Compression of nerves and blood vessels leads to protective muscle spasms that, as the disease progresses, become the cause of pain.

Which doctor treats this disease?
Treatment of osteonecrosis is the field of activity of neurologists. However, when symptoms of osteonecrosis of the neck appear, it is possible to consult a general practitioner. The neurologist will select the drugs for cervical osteonecrosis that are the least stressful on the body, which is important for drug treatment.
To determine the presence of a pathological process in the cartilaginous tissue and tarsal osteonecrosis, the patient is referred for a comprehensive examination. Strategies for the treatment of cervical osteonecrosis are being developed in line with research findings.
Interdisciplinary collaboration also allows the treatment of comorbidities that the patient has. In addition, patients are also supported with full information: treatment protocol, extract service costs, provide specialist advice and diagnostic measures.
Reason
Cervical fibroids develop under the influence of many provoking factors. There is no definite cause of cervical osteonecrosis. The disease is often associated with metabolic disorders and aging of the vertebrae.
Researchers suggest that cervical osteonecrosis develops for the following reasons:
- Excessive stress on the spine. When wearing the wrong shoes, flat feet, obesity, sitting for a long time;
- Metabolic disorder. Vitamin and mineral deficiencies, calcium metabolism disorders can be the cause of degenerative processes in the vertebrae;
- Congenital and acquired malformations of the spine and ligamentous apparatus (ligament thickening, muscle atrophy, ossification);
- Diseases of the gastrointestinal tract, leading to insufficient absorption of nutrients;
- Infection, intoxication;
- Injuries, bruises, fractures of the spine, as a result of which the blood supply and nutrition of the spine is interrupted, are the causes of dystrophy of the spine;
- Stress;
- Wear high heels;
- Pregnancy, especially multiple pregnancies;
- Autoimmune lesions of the connective tissue, structural abnormalities of collagen types 1 and 2;
- Occupational hazards (heavy lifting, prolonged shaking, working in a sitting position with head tilted continuously);
- Atherosclerosis and other changes in the vertebral arteries;
- Curvature of the spine (scoliosis, scoliosis, scoliosis).
An important risk factor for the development of cervical osteonecrosis is genetic burden. This fact proves the presence of osteonecrosis in children, when the spine is not already overloaded.
Degree
Due to the special structure of the spine, it can perform its functions. The main structural unit is considered the spinal movement segment (VMS). It consists of two adjacent vertebrae, a disc and a musculoskeletal apparatus. Osteochondrosis leads to a degenerative degenerative process, first in the discs, then in the vertebrae. With the loss of one vertebra, the performance of its functions is provided by the adjacent vertebrae. This leads to increased load and loss of mobility of the affected segment.
In the development of cervical osteonecrosis, doctors distinguish several stages:
- First degree of cervical osteonecrosis. Since the disc is deprived of its blood supply and nutrients from surrounding tissues, it will undergo degenerative changes. Osteochondrosis in the first stage of development is characterized by destruction of the nucleus pulposus and cracks in the annular fibers. Clinically, this is manifested by acute or persistent local pain in the neck (cervical pain) and stiffness;
- Cervical osteosarcoma grade 2. At this stage, destruction of the annulus fibrosus continues, pathological mobility and instability of the vertebrae appear. The patient complains of neck pain, which is aggravated by exertion, by tilting the head or in a certain position;
- The third stage of the disease is characterized by complete destruction of the ring fibers. The gelatinous kernel is not fixed. Herniated discs can occur and cause severe pain. At this stage, due to poor fixation of the SMS, curvature of the spine can form;
- In the fourth stage of the disease, the intervertebral disc is replaced by connective tissue, other adjacent segments are affected. Spinal degeneration, arachnoiditis develops. The joints become completely immobile - stiffness develops. Bone tissue grows around the affected area - a bone is formed. With the fourth degree of cervical osteonecrosis, vivid symptoms are observed: severe pain radiating to the arm, sternum, to the area between the shoulder blades, sensitivity disturbances.

Symptoms and signs
Signs of cervical spondylosis in the early stages may be non-specific: dizziness, headache, weakness, crunching when moving the head. As the disease progresses, the following symptoms develop:
- Severe pain in the neck and shoulders;
- Hand numbness;
- Dizzy;
- Hypertension;
- Impaired coordination of movements;
- Increased sweating.
There are several syndromes that appear with the development of a pathological condition of the muscles of the back and cervical spine:
- Cervical migraine syndrome.
- Vertebral artery syndrome.
- Hypertension syndrome.
- Heart syndrome.
- Lens syndrome.
They occur when nerve endings are injured and arteries and veins are compressed during the development of the disease. The most dangerous complication is considered vertebral artery syndrome. There is a violation of blood flow through the arteries that feed the brain and spinal cord. Patients with hearing loss, vision loss, constant dizziness. The patient may lose consciousness while driving due to severe impaired blood flow.
Due to the compression of the nerves responsible for the development of the chest muscles and diaphragm, pain in the heart area appears, which is not associated with heart disease, but at the same time, tachycardia, arrhythmia and hypotensionBlood pressure can develop, build up. Compression of the veins leads to the development of CSF hypertensive syndrome. Increased intracranial pressure, nausea, vomiting and severe headache due to decreased blood flow from the brain.
As a result of strangulation, lens syndrome develops - severe pain appears in the neck, shoulders, shoulder blades and back of the head. With this syndrome, the arms and neck area become numb. With migraine syndrome, patients are worried when they have severe pain in the occipital region, often accompanied by feelings of nausea and vomiting.
The reflex syndrome occurs when the spinal roots have not been affected. The patient complains of pain in the neck, head (especially the back of the head), in the arms on one or both sides. Reflex pain, unlike lens pain, is not associated with sensitivity disturbances. Cervical pain can be dull, aching. Sharp "low back" pain is called lumbago. There is muscle spasm and pain, pain in the vertebrae. Signs of tarsal osteosarcoma intensify in an uncomfortable position, with head tilt, coughing, and physical exertion. Signs of spondylolisthesis, periarticular degeneration and shoulder-hand syndrome appear due to nerve impulses from the annulus fibers of the affected segment, causing compensatory muscle spasms.
Lens syndrome is associated with impaired motor activity and sensitivity. At the same time, the nerves, blood vessels are impaired, and the outflow of veins and lymph in the pathological focal point is disturbed due to the impaired intervertebral canal. Pain in lens syndrome is acute, intense. A common cause of spinal nerve compression is the formation of a hernia. In the area of pathological focus, muscle tone is reduced. With ischemia, in addition to the nerves, the vessels are compressed.
If the phrenic nerve is involved in the pathological process, cardiac syndrome occurs. Manifestations are burning, acute pain in the left chest when radiated into the arm, sternocleidomastoid muscle. The name of the syndrome is due to the nature of the pain that is similar to an angina attack. The main difference between the pain in angina is that it is relieved after taking nitroglycerin, it can occur at rest and is associated with heart rhythm disruption (tachycardia, arrhythmia).
Signs of cervical osteonecrosis depend on the localization of the pathological process. With damage to the upper cervical vertebrae, the blood supply to the brain is interrupted because the cerebral arteries are compressed. This leads to headaches (especially in the occipital region), dizziness, fainting, high blood pressure. Dizziness with cervical osteochondrosis is caused by decreased blood flow to the inner ear. Patients are also worried about nausea, vestibular and ocular symptoms.
With a combined lesion of the vertebrae, they refer to tarsal osteonecrosis. The disease is manifested by the following symptoms:
- Dizzy;
- Pain in the neck and arms;
- Tingling, crawling sensation in the upper extremities;
- Intercostal neuralgia.
Diagnose
Cervical fibroids are a chronic disease that can lead to the formation of herniated masses and spinal cord compression. Therefore, it is important to establish the correct diagnosis promptly and initiate treatment. To identify cervical osteonecrosis, the following types of instrumental diagnostics are used:
- Spine scan or X-ray of the spine. This research method is painless, informative, and requires no special training. X-rays of the spine allow you to evaluate its anatomical and functional features. In the photo, attention is paid to the structure of the vertebrae, their relationship to each other, the distance between them, the lumen of the spinal canal;
- Computed tomography - provides information mainly about the state of bone tissue, allows you to identify spinal stenosis and herniated discs;
- Magnetic resonance imaging - allows you to identify changes in soft tissues. MRI images clearly show changes in the discs and spinal cord.

Medicines for treatment
Treatment of cervical spondylosis with drugs and without drugs. Even after complete cure, neurologists still take precautions to rule out recurrence of the disease. In the acute stage, for the treatment of cervical spondylosis, the doctor prescribes the patient drugs of the following pharmacological group:
- Non-narcotic pain relievers. They are taken orally or intramuscularly to quickly achieve an effect;
- Non-steroidal anti-inflammatory drugs;
- B vitamins in large doses.
Diuretics are used to reduce water retention in the spinal roots and surrounding tissues. Antihistamines increase the effect of pain relievers. Muscle spasms are eliminated by muscle relaxants. With persistent severe pain syndrome, neurologists perform nerve blockade.
To improve metabolism in the intervertebral disc, people use chondroprotectors. These drugs increase the content of glycosaminoglycans, increasing the firmness, elasticity, and shock absorption of the disc.
Dizziness medicine
Patients often experience dizziness with cervical osteonecrosis. To relieve them, doctors prescribe non-steroidal anti-inflammatory drugs. NSAIDs belong to different classes that differ in their mechanism of action and action, so only a qualified specialist can determine the appropriate drug.
It is important to remember that cervical spondylosis cannot be used without a prescription from your doctor. Non-steroidal anti-inflammatory drugs have side effects, therefore, before prescribing, the neurologist determines the presence of contraindications in the patient and the required dosage. Drugs for the treatment of vertigo in cervical osteochondrosis can improve a patient's quality of life.
Injections for osteonecrosis disease
Injecting drugs to treat cervical spondylosis help relieve pain during an acute attack. With this method of drug administration, the effect occurs quickly. Neurologists use a variety of injectable drugs.
The nurse injects the drug solution under the skin, intramuscularly, or intravenously. In the period of exacerbation of the disease, drugs used parenterally, with the method of cervical osteolysis, have only symptomatic treatment.
Headache treatment
Headache is a symptom that occurs with many different disorders. However, cervical osteonecrosis is characterized by severe headaches. Head movements increase symptoms, therefore, to eliminate it, doctors prescribe pain relievers and non-steroidal anti-inflammatory drugs.
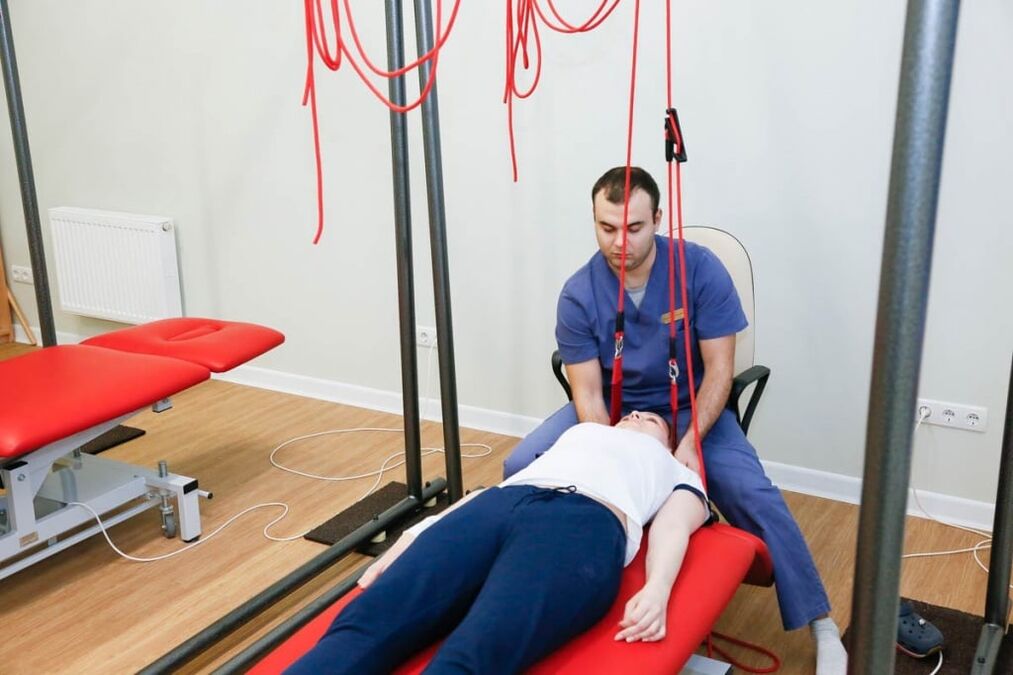
Non-drug therapies
Complex non-drug therapy for cervical osteochondrosis includes:
- Protective mode - when the roots are pinched, the patient lies on a hard surface,
- Massage;
- Physical therapy exercises;
- Spinal traction;
- Physiotherapy procedures.
Cervical spondylosis massage is used to relieve pain and swelling, improve peripheral blood supply, and eliminate muscle spasms. A contraindication to performing this procedure is the presence of acute pain. Massage your neck and back in the direction of lymph flow. Pay special attention to the intervertebral and vertebral regions.
Gymnastics for cervical spondylosis is aimed at eliminating muscle spasticity and strengthening the muscular frame. Since instability of the vertebrae often occurs in the cervical spine, the physiotherapist conducts individual lessons in which he instructs the patient to perform the exercises safely. . Some authors recommend conducting physical therapy classes in the Shants collar.
To improve mobility of the cervical vertebrae, rehabilitation therapists recommend the following exercises:
- Curvature and extension of the neck. Tilt your head forward toward your sternum, without pulling your shoulders forward, then back. Hold the side position for 3 seconds, repeat each exercise 8-10 times;
- Turn your neck. Turn your neck first to the left until it stops, then to the right, without changing the position of the shoulders and the level of the chin;
- Keep your head down until you stop. Then tilt your head back without changing the level of your shoulders. Hold the pose for 5 seconds.
The following exercises have been developed to strengthen the muscles of the neck:
- Place your hands behind your head. Tilt your head back, put it on your hands;
- Place your hands on the temples. While tilting your head, counter with your hands;
- Place your hands on your forehead, resist, tilt your head forward;
- Tilt your head to the side with your right hand, with your left hand behind your back. Repeat the exercise on the other side.
Self-gravity therapy is the correct name for spinal traction. It is done using special equipment. The goal of therapy is to reduce muscle spasms and restore the correct position of the vertebrae. To avoid complications, a spinal traction is performed by a doctor.
To improve blood supply in the pathological area, reduce puffiness and eliminate pain, the following physiotherapeutic procedures are used:
- Diadynamic series. During this procedure, using a special device, a low-frequency electric current is applied, stimulating the muscles, reducing spasms and pain. Has a positive effect, improves the thermal properties of tissues;
- Ultraviolet irradiation. Under the influence of UV radiation, vitamin D metabolism is improved, calcium content increases, bone tissue is stronger;
- Ultrasonic wave exposure - used for blood flow acceleration, antispasmodic and comparative action. Ultrasound can penetrate deep into tissues, sometimes it is used for better drug absorption;
- Amplipulse therapy - allows you to relieve pain by blocking nerve impulses from the painful area.
In the acute stage of the disease lasting from 4-7 days, use analgesics, antispasmodics, and reduced stimulation to relieve pain. The patient is provided with peace. Cervical spine immobilization is performed by Shant collar. Exercise therapy and massage are contraindicated. Apply UV radiation.
The duration of the subacute phase is 29 days. After complete recovery, the patient must rest for a few days. You can then begin a course of rehabilitation therapy. In the chronic stage of the disease, the patient is prescribed muscle relaxants, chondroprotectors, B vitamins, analgesics, NSAIDs. Physiotherapy exercises, massage are provided. The patient underwent physical therapy (amplipulse, alternating current exposure), performed spinal traction.

Dish
Proper nutrition for osteonecrosis is an important condition for remission of the disease. The progression of tarsal osteonecrosis stops with diet and treatment. Neurologists know how to treat cervical spondylosis, so they create a complex of treatments that include procedures, exercise therapy, proper nutrition, and replacements. lifestyle change.
Many patients turn to neurologists with the question of how to treat cervical spondylosis and whether there are any dietary restrictions. Therapists create individualized nutrition programs that take into account patient preferences. The osteosarcoma diet is based on foods that are balanced, low in fat, and rich in nutrients. The patient's daily diet includes foods high in calcium.
How to sleep with cervical osteonecrosis
For patients with diseases of the musculoskeletal system, the question of how to sleep properly with cervical spondylosis. Sleeping on your stomach makes the disease worse, so it's better to avoid sleeping in this position. The most optimal positions are on the back and sides.
Cervical fibroids develop while resting on a soft mattress. Therefore, experts recommend giving preference to elastic mattresses, as well as pillows of moderate softness. If a patient is diagnosed with cervical osteosarcoma, experienced therapists will tell you what type of bed is safe to sleep in.
Preventive
To prevent the onset or progression of cervical osteochondrosis, doctors recommend:
- Maintain correct posture;
- Having an active lifestyle, resting at work;
- Perform regular physical therapy exercises;
- Sleep on firm and flat surfaces, orthopedic mattresses and pillows;
- Quit bad habits, especially smoking;
- Choose shoes taking into account the physiological structure of the foot;
- Do not carry a bag with one hand, this leads to spinal curvature;
- Follow a healthy lifestyle, eat right, eat lots of fruits and vegetables;
- Do not sit for a long time with the head tilted;
- Swim.
To improve blood circulation, massage therapy should be done regularly.






























